- +91 99202 00400 / +91 22 4113 6565
- contact@neurogen.in
Disclaimer: At NeuroGen BSI, autologous bone marrow tissue, after minimal manipulation, is grafted by medical practioners as part of routine procedure within the hospital in the same surgical sitting. According to the directives of the Ministry of Health and Family Welfare issued under section 33P of the Drugs and Cosmetics Act,1940 this procedure does not involve use of stem cells/ stem cell derived product.
Cerebral - of the brain, Palsy: lack of muscle control
Cerebral palsy is an umbrella term that refers to a group of non-progressive brain injury or malformation disorders that affect a person's ability to move.

It happens due to damage to the developing brain either during pregnancy or soon after birth.
Children with cerebral palsy may also have visual, hearing, speech, learning, epilepsy and intellectual problems.

Based on affected region:
Monoplegia : affects one limb, usually an arm
Hemiplegia : affects one side of the body including arm, leg, and trunk
Diplegia : affects either both the legs or both the arms
Quadriplegia : affects all four limbs
Based on Clinical Presentation:
Spastic Cerebral Palsy : Tightness in the limbs involved.
Dyskinetic Cerebral Palsy : Involvement of Excessive Involuntary movements. Can be either:
Dystonic : Alternating between rigidity and flaccidity.
Choreoathetoid Cerebral Palsy : Constant involuntary movement leading to abnormal postures.
Ataxic : Involvement of the cerebellum (smaller brain).
Mixed Cerebral Palsy : Involvement of different parts of the brain.
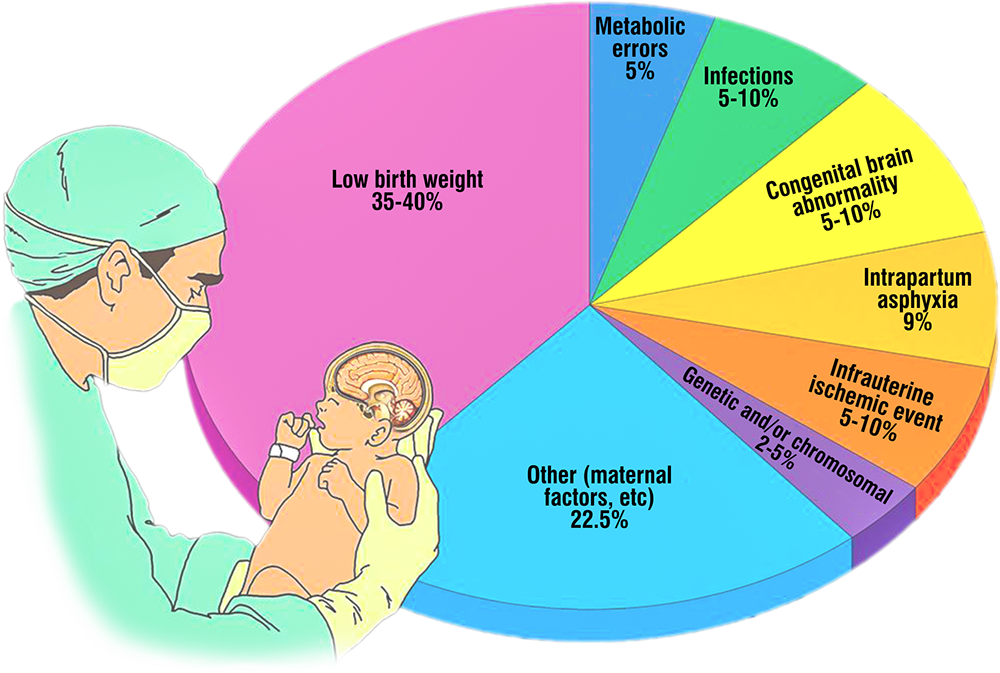
Cerebral palsy may occur due to any kind of abnormality in brain development, either while the fetus is developing inside the mother's womb, or due to a brain injury (traumatic or hypoxic) or infection during birth or soon after birth, leading to brain damage.




reduction in the baby's blood or oxygen supply
an infection caught by mother such as cytomegalovirus, rubella, chickenpox or toxoplasmosis
an injury to the unborn baby's head
genetic disorders such as Down's Syndrome, Rett Syndrome
asphyxia: lack of oxygen to the brain during a difficult birth
an infection of the brain such as meningitis
a serious head injury during forceps/suction delivery or after birth due to external trauma
choking or nearly drowning, causing lack of oxygen to the brain
a very low blood sugar level
a stroke: sudden blockage of blood flow to the brain
Prematurity (birth before the 37th week of pregnancy): babies born at 32 weeks or earlier are at a high risk since the fetus has not grown completely
a low birth weight
a twin or multiple pregnancy
the mother being 35 years of age or older
the mother having unusually low blood pressure or high blood pressure
Bacterial and viral infections
Prenatal exposure to drugs and alcohol, stress, heavy metals including mercury poisoning from fish

The earliest sign of cerebral palsy is delayed development. Basic motor milestones such as sucking, neck control, rolling, sitting without support, crawling, grasping, etc. are observed to be delayed, with a high chance of low body weight.
One of the early signs, due to lack of muscle tone, in children with Cerebral Palsy, is the ‘floppy body’ commonly called, hypotonia. Sometimes, an abnormal muscle tone can also be seen in the form of stiff or rigid muscles.
Depending on which part of the brain has undergone damage, the child may use only one side of the body more than the other, while reaching for things, crawling, or moving.

Child hands in upside down 'U' with little or no movement.
Head drop

Body stiffens like a board
Arching of trunk
Twisting of legs
Specific to age, the early signs of Cerebral palsy in infants can be observed in the following way:
Younger than 6 months of age:
Lack of Neck Control when picked up
Weak sucking or tongue thrusting
Abnormal muscle tone; stiff or sloppy
Stiffening of lower limbs, this creating a crossing or a scissoring appearance of lower limbs
Apparent overextension of their back and neck, making it look like they’re pushing away from the person lifting them
Older than 6 months of age:
Lack of rolling ability
Difficulty in moving upper limbs or bringing them together
Crawling in a lopsided way, with dragging the other side of the body
Unable to stand or walk without support
Doesn’t respond to own name
Doesn’t babble
Doesn’t say words like ‘mama’, ‘papa’, etc.

Excessive lethargy or irritability or high pitched cry

Poor head control

Weak suck/Tongue thrust/Tonicbite/feeding difficulties
Commonly, the physical symptoms of Cerebral Palsy, are manifested with age, and usually as a result of lack of appropriate rehabilitation.

Physically, the symptoms which may arise, could be deformities, of the upper and lower limbs causing a bent wrist, or a closed fist, or a rigid flexed elbow. These usually affect the grasping and holding capacity of the patient, leading to a poor grip. Due to a generalised delayed development, there could be severe malnourishment, with a floppy body, commonly known as hypotonia. The deformities or rigidity which may occur in the lower limbs, could result in difficulty in walking.

The physical symptoms may range from a lack of balance or a scissoring gait while walking, to difficulty in breathing, which may need ventilatory support. The difficulty in breathing often occurs as a result of not only a poor neck control, but also, due to lowered immunity. Often, children with cerebral palsy face recurring chest infections due to aspiration pneumonia. This happens due to poor swallowing and poor neck control, which could lead the oral intake of food to enter the trachea and thus irritate the respiratory tract and increase the risk of infections.
Very often, children with Cerebral palsy also face issues sensory issues such as poor vision and poor hearing, along with cognitive difficulties. They may have issues of intellectual disability or delay.
Due to a lack of tone in general, they may have excessive drooling as well. As a result of brain damage, children with Cerebral palsy may often experience seizures or epileptic attacks, which needs immediate medical intervention. Some children with Cerebral palsy also face issues of hydrocephalus, which is an excessive fluid accumulation around the brain, thus causing a pressure to the skull, leading to an increased head circumference.
Associated Symptoms of Cerebral palsy
These are the symptoms of Cerebral palsy, which may not necessarily occur in all such children, however, may often be a result of the core symptoms of cerebral palsy. These may include pain due to the joint rigidity, hip displacement as a result of hypotonia, non-ambulation due to lower limb deformities or lack of strength, speech difficulties, epilepsy, behavioral changes due to lack of intellect, poor bladder control, disturbed sleep cycles due to breathing issues, vision and hearing impairments, and a difficulty in swallowing.

A physiotherapist is trained to diagnose, manage and treat the symptoms and movement restrictions that are accompanied by Cerebral palsy. The exercises which are formulated and advised by physiotherapists are meant to enhance the physical and functional skills of the child with Cerebral palsy. Physical therapy when monitored and given systematically and regularly, can help prevent physical complication, deformities and disabilities which form as a result of Cerebral palsy. This promotes an overall well-being, health and fitness, thus, facilitating an improved quality of life.




Currently there is no cure for cerebral palsy. Treatments available help in minimizing the symptoms, preventing future complications, and maximizing functional independence.
A multidisciplinary approach is being followed to achieve the above goals. This includes:
Physiotherapy is one of the most important treatments for cerebral palsy.
Physiotherapy helps to increase strength of weak muscles, encourage movement, lengthen the tight muscles, prevent contractures of muscles, alleviate pain, thereby enhancing mobility and maximizing independence. Physiotherapists use techniques such as NDT, Bobath, Rood's approach, stretching, gait training, selection of appropriate aids and orthosis to achieve the above goals.
Occupational therapy as the name suggests, is the identification of the problems that a child faces in day to day tasks and to addresses them so as to make the child enable to carry out complex movements involved in daily tasks such as bathing, dressing, transferring to the toilet, etc. Also, parents and caregivers are educated for possible modifications which can be done to assist the child in a functional activity. Thus occupational therapy helps boosting children's and parents' self esteem and confidence, which in turn helps the children to become independent with their daily activities.
Children with cerebral palsy may have difficulty in speech and language development, and many a times experience difficulty with facial expressions and hand gestures. Speech therapy thus aims at improving oral motor skills, speech and language skills. Children who cannot speak, are taught sign language, or how to use special equipment like computer/tablet for communication through pictures, etc. A speech therapist also provides guidance regarding hearing aids if hearing deficit is the cause of delayed speech.
Children with cerebral palsy may also suffer from chewing and swallowing difficulties due to weakness of masticatory (chewing) muscles and pharyngeal (swallowing) muscles. Difficulty in swallowing can be life threatening since it can cause severe choking or food entering the windpipe causing difficulty in breathing, or it can cause aspiration pneumonia of the lungs resulting in long term ailments and malnutrition. Thus a speech therapist teaches children and caregivers swallowing techniques, appropriate positioning and oro-motor exercises, makes dietary changes as in the consistency of food (soft/liquid/mashed), etc. In more severe cases, a feeding tube has to be inserted into the stomach through the nose or directly into the stomach through the skin of the abdomen by a trained gastroenterologist.
Medications are given to children with cerebral palsy to manage their difficult to manage symptoms such as seizures, spasticity, dystonia, pain, drooling, etc which come in the way of child's development and the therapy. Parents have to get a consultation from a pediatric neurologist or pediatrician for medical assistance.
Following are few examples of common symptoms and medications advised:
Seizures: carbamazepine, phenytoin, valproate, valproic acid, gabapentin, lamotrigine, levetiracetam, topiramate, etc.
Spasticity: baclofen, clonazepam, dantrolene, diazepam, etc.
Dystonia: levodopa, procyclidine hydrochloride, diazepam, lorazepam, clonazepam
Pain: acetaminophen, ibuprofen
Drooling: Glycopyrrolate
Constipation: Dulcolax, magnesium hydroxide, lactulose
Behavioral problems: medications for ADHD,
Children with cerebral palsy may develop contractures of muscles resulting in limited joint range, joint and bony deformities such as scoliosis, dislocation of hip, etc which need corrective surgery like tendon release, corrective osteotomy. These surgeries are performed by pediatric orthopedic surgeons.
The treatment options that are currently available help the patients in managing the symptoms to some extent, but they do not repair the underlying brain damage. Therefore developing a standard therapeutic approach is a need of the hour. Scientists and researchers worldwide are now considering regenerative medicine as a potential treatment option for patients suffering from cerebral palsy.
Till very recently, it was believed that brain damage during birth is irreversible. However, now with emerging research, we understand that it is possible to repair the damaged brain tissue using regenerative medicine.
Cell obtained from various sources can be used for regenerative medicine. Our approach, at NeuroGen BSI makes use of autologous bone marrow derived mononuclear cells (BM MNCs) for transplantation. The transplanted cell have the ability to migrate to the area of the damaged tissue in the brain and home in those affected areas to help repair the damage. They release several trophic factors that decrease the effects of damage in those areas and also differentiate into several cell types of the nervous system such as oligodendrocytes, glial cells and other cells of the nervous system. The main mechanisms that help tissue repair and regeneration include:-
Prevention of cell death in neuronal population
Establishment of new blood vessels
Cell multiplication and integration
Establishment of new neuronal maps in the brain in order to learn new functions.
These mechanisms repair and regenerate the damaged tissue, restoring activity in the affected area, which translates into clinical improvements .This plays a great role in improving the overall quality of life. Also autologous BM MNCs do not show any adverse side effects and they do not face any immune rejection. Also, they are obtained from the same patient and thus are free of the ethical issues surrounding the use of cell.
With our comprehensive approach and our aim to guide and support our patients through thick and thin, we have successfully treated over 1400 patients with cerebral palsy. The patients who had reached a plateau stage, after regenerative medicine have shown colossal improvements in their symptoms. Most of the symptoms that are seen in cerebral palsy are oromotor /speech, balance, trunk activity, upper limb activity, lower limb activity, muscle tone and ambulation. Together, they affect activities of day to day life.
We analysed the effect of regenerative medicine in 1400 patients diagnosed with cerebral palsy. Changes in common symptoms like oromotor/ speech, balance, trunk activity, upper limb activity, lower limb activity, muscle tone, ambulation and Activities of Daily Living were recorded on follow up. The improvements were graded as no change, mild improvements, moderate improvements and significant improvements. Analysis revealed that out of approximately 1400 patients, overall 91.01% patients showed symptomatic improvements and approximately 8.98% of patients showed no improvements in any of the symptoms.
Overall 91.01% patients showed symptomatic improvements
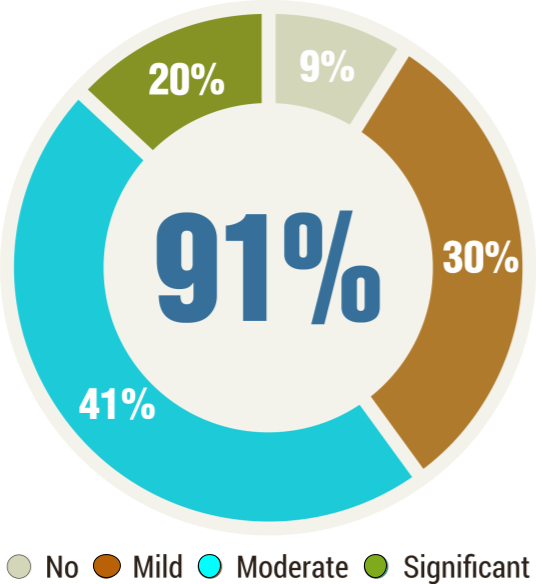
Mild improvements were observed in 29.96% of patients, moderate in 41.19% of patients, whereas, 19.85% of patients showed significant improvements. We observed that patients who continued regular exercise program at home under supervision of professional therapists showed significant improvements. Patients who did not follow regular rehabilitation showed mild improvements. Therefore, in our experience regenerative medicine should be followed by regular rehabilitation under supervision of a therapist.
The positive changes that we record in our patients are not just restricted to their symptomatic improvements, but also bring about a constructive change in their brain metabolism as observed in their PET-CT scans.
Objective radiological evidence of improvement in patients with cerebral palsy
Intrathecal autologous regenerative medicine is safe, feasible and effective treatment strategy for children with cerebral palsy. This repairs the underlying brain damage which can also be objectively seen on PET CT scan of brain along with improvement in functional and achievement of milestones in children. regenerative medicine along with standard treatment augments the development and improves the quality of life of these children.


Cerebral Palsy refers to a permanent condition and problems related to this condition remain throughout the patient's lifetime, however, these children can cope up with the condition as they grow. Various treatments available often bring out significant improvement in the condition, however, cannot cure it.
No. Your child's condition will not deteriorate further unless there are any underlying factors such as any illness or infection which may cause the child's progress to come to stand still.
Stiffness in the muscles is due to spasticity, contractures or both. It is difficult to distinguish between spasticity and shortening and during growth spurts the child's bones will grow more rapidly than muscles, which lead to tightening and activities like walking or standing makes it more apparent. Treatment for spasticity and shortening is different.
Yes it can, especially when the child is pushed or forced to achieve a skill, they may react by becoming stubborn or may refuse to cooperate, and this may certainly be a reason for lack of progress but which actually does not mean that the child's condition is deteriorating. But if the child loses previously acquired skills, then it is important that you should discuss it with your therapist or doctor.
Every child with cerebral palsy is different, and so it is not possible to come to a conclusion, unless the child has been observed over time by the pediatrician and therapist. As parents you are always curious and worried about your child's walking. However, children with mild cerebral palsy can learn to walk independently, children with moderate cerebral palsy may walk with a stick or walker and children with severe cerebral palsy are generally wheelchair-bound.
Yes and no. Most children with cerebral palsy may not have any difficulty in talking, while a few may have difficulty in controlling the movements around the mouth or delay in developing learning skills. Children with cerebral palsy will need help from a speech therapist to learn how to use alternative methods of communication or develop speech.
The aim of all treatments is to encourage these children to learn to be as independent as possible. As parents it is always important for you to encourage your child to do as much as possible. Children with mild cerebral palsy may not have any problems achieving independence but the ones with severe cerebral palsy may require assistance from others throughout their lives.
Some children with cerebral may have behavioral problems, which can be difficult to manage. They may also be frustrated, due to inability to move, talk. Clinical psychologists play an important role in addressing behavioral issues and help develop and motivate and encourage child to feel good about them and be happy.
Most children with cerebral palsy are healthy and lead a normal life. Children with severe brain damage associated conditions such as epilepsy may be a risk of reduced life expectancy.
It is extremely unlikely for your second child to have cerebral palsy. Please ask your doctor to guide you about genetic counseling and future care in pregnancies.
Bone marrow transplantation has been used successfully for genetic disorders of blood, such as sickle cell anemia, thalassemia, as well as cancers such as leukemia. Since our therapy uses these very cell, which are harvested from the patient's own body (autologous cells), there are no major ethical concerns. Ethical concerns are primarily on the use of embryonic cell (which we do not use).
Bone marrow transplantation has been used successfully for genetic disorders of blood, such as sickle cell anemia, thalassemia, as well as cancers such as leukemia. Since our therapy uses these very cells, which are harvested from the patient's own body(autologous cells), there are no major ethical concerns. Ethical concerns are primarily on the use of embryonic cell (which we do not use).
In case of children with seizures, or previous history of seizures or an abnormal EEG, a small possibility of triggering seizures can be there. However, proper antiepileptic cover/drugs, could circumvent this problem.
Maximal improvements are seen around 3-6 months after the treatment. However, in many patients there are slow progressive improvements that continue for several months/years later. Most patients do show some immediate improvements also i.e. before the discharge, in some of their symptoms.
The decision to do the therapy a second time is taken after seeing the progress/improvements after the first therapy. A complete assessment will be done by the rehabilitation team, certain special imaging tests, such as PET CT Scan of the brain, would be repeated and then a second treatment may be recommended. This may be done anytime between 3-6 months of the first therapy.
We will review what other medications the patient is already on. In most cases, we do not discontinue any already going on treatment. However, this is decided on a case by case basis. Please inform us about any medications you are taking beforehand.
Master AY, a 5 years old male child, is a known case of Diplegic Cerebral Palsy. His chief complaints were drooling, unclear speech, difficulty in standing and walking without support, poor hand functions of left arm, affected coordination, poor sitting and standing balance, Improper Gait, tightness in arms and legs, poor cognition, etc. Like every parent Mast. AY's family consulted many allopathic and homeopathic doctors from different parts of India. However, everyone they consulted with, said nothing substantial could be achieved, which diminished their hope, each time. Mast. AY used to go for physiotherapy but not on a regular basis. "In a local function we met a family having a child like AY and that family told us about NeuroGen Brain and Spine Institute in Mumbai, so we immediately started our search. I went through their website, spoke to Dr. Nandini Gokulchandran on phone about my child's case and decided to take AY to NeuroGen for Regenerative Medicine." said the father.
AY came to NeuroGen in August 2015, where he underwent Regenerative Medicine along with a customized rehabilitation program which aimed at increasing the strength of affected areas, improving dissociations, posture, balance, walking, grip, cognition, and increasing overall stamina of the patient. The family found new hope with NeuroGen's Regenerative Medicine and were motivated and positive for their child after going back home and they continued with his rehabilitation.
There were tremendous improvements seen in AY's condition during their follow-up in December 2015:
His attention had improved; he paid attention towards things that interested him.
Cognition had improved, started identifying few colors, alphabet 'A'.
Memory became better.
Lying, sitting and standing posture had improved.
Crawling was better. Weight shifts had improved in walking.
Neck holding had improved.
Sitting static balance had improved from fair to good.
Standing static balance had improved from fair to good.
Walking static balance had improved.
Holding objects with his hands, fisting & opening his hand had improved compared to earlier.
Walking pattern had improved and knees were straight now.
Foot movement had improved from poor to fair.
He was able to assist his mother in grooming himself, with upper body and lower body dressing.
Sitting was better than before (more erect). Sitting in 'W' posture was lesser.
Standing posture was better.
Kneeling had improved.
He tried to pick up objects from floor.
Tightness had reduced (lower limb more than upper limb).
Balance had improved. Had started walking independently without support.
Drooling had reduced.
He could drink water by using both hands better than before.
He could eat with spoon better than before.
Handwriting had improved. Earlier, he used to scribble, now he could write better than before.
Floor to bed transfer was better. He could climb up on bed with support now.
Life of this resilient child, AY, has changed after Regenerative Medicine. He can play a little better, understand better, he can enjoy his childhood a little better. They went ahead with the second dose of regenerative medicine in March 2016 with the hope of him attaining near normalcy. "After consulting many doctors and hospitals my search finally ended at NeuroGen BSI where we got great positive results. Today we are more positive, motivated and very well guided in our path to help our child recover. I would suggest all parents like us should at least go to NeuroGen BSI (Mumbai) once." said his father.
Master DJ, 5 year old boy from Vijayawada is a known case of Diplegic Cerebral Palsy. " Our major concerns for DJ were his delayed milestones and thanks to our family and their support, we did not let the reality affect us and started looking for various treatment options." In April 2016 his Physiotherapist asked his parents to check Regenerative Medicine at NeuroGen Brain & Spine Institute, Mumbai. DJ's parents found new hope for development of their son. Without any further they decided to go ahead with regenerative medicine for him in May 2016.
DJ's complaints according to his parents were inability to transfer from one place to another, stooped sitting, tightness in legs, thighs, calves, difficulty in crawling, inability to stand and walk independently, difficulty in gripping objects, cognition and problem solving not age appropriate, inappropriate eye hand coordination.
At NeuroGen, he underwent Cell Treatment followed by intensive neurorehabilitation which included physiotherapy, occupational therapy, cognitive and behavioral therapy, special education which aimed at reducing spasticity and tightness, improving movement control, gross and fine activities, problem solving, etc.
Following were the improvements seen in DJ's condition six months post Regenerative Medicine
Sitting posture had improved. He could sit in an erect manner now.
His balance as well as reaching out for things had improved.
He could walk with one hand support, which wasn't possible earlier.
He could now do side walking minimum 5 steps each side with 2 hands held.
Higher mental functions had improved. He could now follow more commands at a time.
Grip in left hand had improved and tightness had reduced.
Walking pattern had improved.
He had started bathing by himself and brushing by himself.
Overall tightness of the body had improved.
DJ had now started going to school. "Our experience at NeuroGen BSI was good, we are satisfied with the guidance we got, the doctors and the entire support staff are very helpful. regenerative medicine has given that push in his progress and a hope in our minds that he will soon start living an independent life. Looking at DJ getting so much love from everyone who meets him is very motivational for us," concludes his father.